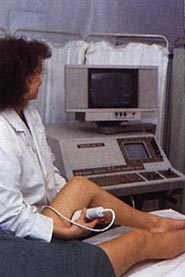
 If you have a persistent bad calf cramp it could be indicative of a blood clot. A blood clot, once in your body, can break off, go elsewhere and get into your lungs and/or brain and kill you. I did not know this a year ago, and even after the clot went away after six months of medication, it does not seem to be as widely, or as clearly stated, as it should be.
If you have a persistent bad calf cramp it could be indicative of a blood clot. A blood clot, once in your body, can break off, go elsewhere and get into your lungs and/or brain and kill you. I did not know this a year ago, and even after the clot went away after six months of medication, it does not seem to be as widely, or as clearly stated, as it should be.
“Your life is in danger – this is an urgent medical condition.” On June 10, 2015 I heard that statement many times from medical professionals and would continue to hear it often as the DVT diagnosis, treatment and resolution continued over the following six months.
Persistent calf pain, which felt like a standard athletic cramp, had driven me to the first of several physician appointments which led to the diagnosis. If you are experiencing such a cramp, or have had a persistent issue with your calves, you may be experiencing a DVT.
Chris Bosh had a much worse condition that included clots traveling to his lungs, which can lead to an embolism. Women who suffer DVTs through pregnancy and delivery are at higher risk than I was. There are many common ways in which a clot can occur, and my experience was about as good as it could be all things considered. I got off easy – but it was completely new to me that the initial pain could arise from what felt like a conventional athletic cramp.
After multiple appointments with several types of physicians, many risk factors were identified, but none was ever clearly the “smoking gun.”
- Trauma to the leg – I had bumped my front shin against a steel beam 10 days prior to the diagnosis, and trauma is a known risk factor. The migration of this pain, from the shin on the front of my leg to the calf in the back, was one of the m
- Flight – I travel a lot and regularly fly overseas. DVTs are a known complication of long flights with a host of ways to mitigate the risk, including wearing of calf compression socks (which themselves are recommended mostly due to their ability to mitigate pain once someone is diagnosed with a DVT, rather than do to known statistical mitigation of DVT onset). While this is the most widely known factor – most of the physicians I saw did not think this was a major factor.
- Exercise – I had worked out a lot prior to onset.
- Dehydration – Due to the exercise, travel, and a common side effect of me being Celiac.
- Celiac – I’m Celiac, but there is no known data about risk factor correlation between this and DVT. (Although most auto-immune disorders like Celiac tend to make everything worse.)
- Rhabdomyolysis – In 2014, I had exercise induced Rhabdomyolysis (this is its own long story, due largely to Celiac, Exercise and Dehydration). There is some data that there is correlation between this and DVT.
After six months of blood thinners with no change in the size of the clot, the physicians I was dealing with agreed that continuing that therapy was unlikely to be successful. Fortunately, one final ultrasound showed that the clot had greatly decreased in size. I will continue to take a thinner for flights over 5 hours.
Throughout this process there was; (1) a lot of fear, (2) inconsistent information, and (3) not much guidance as to finding others who had had similar experience. Hopefully this helps someone else should they have the same issue develop.



You must be logged in to post a comment.